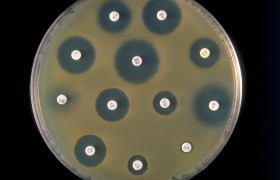
Antibiotic resistance growing global problem for children with urinary tract infection
The prevalence of resistance to commonly prescribed antibiotics in children with urinary tract infections is high, especially in countries outside the Organisation for Economic Co-operation and Development (OECD), according to a recent article in the British Medical Journal. In an editorial, an Australian professor of General Practise Research warns about the drastic consequences of this finding for clinical management.
Ashley Bryce and colleagues reviewed 58 studies on the worldwide prevalence of resistance to antibiotics in primary care in children with urinary tract infection caused by Escherichia coli. In addition, they performed a meta-analysis of five of these studies to determine the relation between previous antibiotics use in primary care and resistance.
The prevalence of antibiotics resistance was higher in non-OECD countries than in countries inside the OECD. For example, the prevalence of ampicillin in OECD-countries was 53 per cent, compared to 80 per cent outside the OECD. Other extremes were co-amoxiclav with 8 per cent in the OECD and 60 per cent outside the OECD and co-trimoxazole with respectively 30 and 69 per cent in- and outside OECD countries. The meta-analysis showed that children who had previously been prescribed antibiotics were more likely to be resistant to them. This elevated risk could persist for up to six months. The authors suggest that the over the counter availability of antibiotics in non-OECD countries might explain their findings.
General practitioner and professor of General Practise Research Grant Russell explains his view on these findings in an editorial. He points to the guidelines that for an antibiotic to be considered a first line empirical treatment for urinary tract infection, resistance should not exceed twenty per cent. The study by Bryce and colleagues shows that this threshold has been reached for many of the commonly used antibiotics. According to Russell, this shows that it is time for a change in the guidelines. He concludes his argument with a rather pessimistic statement. “While I have no doubt that clinical practise guidelines will quickly be able to accommodate these findings, I am less confident that there is the will and commitment to deal with what the WHO has called ‘the post-antibiotic era’.”
Source: BMJ
MedZine writes about notable science twice a week.